On this snow day in New Jersey, I decided to tackle the common topic and procedure of hysterectomy.
As an obstetrician and gynecologist, hysterectomies are a surgical procedure that I routinely perform. In an attempt to demystify this popular surgery, let’s start by discussing what a hysterectomy is.
The medical term “hyster” means uterus. Thus, a hysterectomy is the removal of the uterus. The uterus is the female organ where babies grow.
The lining of the uterus is responsive to hormones released by your ovaries and hence proliferates in response to estrogen and is shed in response to progesterone. This is more commonly known as your period.
Once a hysterectomy is performed, a woman will no longer possess the capability of childbearing, nor will she continue to have menstrual periods.
Reasons Why Women Have Hysterectomies
Fibroids
This is one of THE MOST common reasons I perform hysterectomies. Fibroids are a benign proliferation of smooth muscle. They can cause the uterus to become enlarged.
Fibroids can range in size, from the size of a pea to the size of a watermelon!
Common symptoms usually associated with fibroids include heavy periods, pressure, pain, or sometimes bowel/bladder issues. The latter translates either into the constant sensation of feeling as if you “have to go” or difficulty completely relieving yourself.
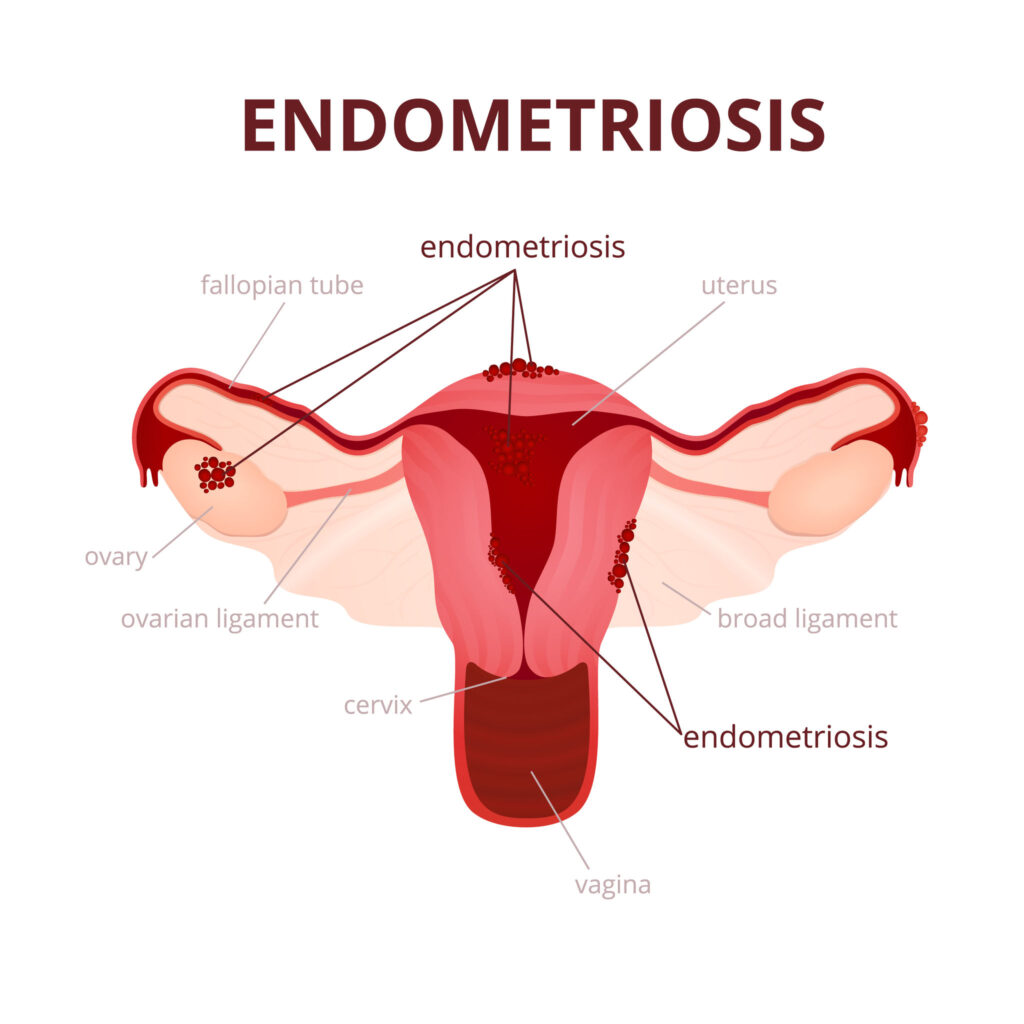
Endometriosis
Endometriosis is a medical condition where the lining of your uterus (as noted above), which is typically shed as your period every month, gets shot out through your fallopian tubes and implants on various aspects of your abdomen and pelvis.
Endometriosis can be seen in the cul-de-sac of your pelvis, your ovaries, and even in unsuspecting locations such as your diaphragm, lungs, bowel, etc.
The characteristic symptom of endometriosis is cyclical painful periods.
Adenomyosis
Adenomyosis is like the first cousin of endometriosis.
What happens with adenomyosis is that the same lining that is typically shed as your period invades the body, or musculature of the uterus. Hence, uteruses become enlarged.
On ultrasound, uteruses will have a bulky appearance without obvious cause; that is, no structural abnormalities such as fibroids.
Women with adenomyosis will complain of heavy painful periods. While changes associated with adenomyosis can be visualized on MRI, adenomyosis is a pathological diagnosis and will be noted on the final tissue reading.
Uterine prolapse
Prolapse is often described by women as having the sensation of “something falling out of their vagina,” or “feeling something down there.”
Prolapse doesn’t kill you, but can cause issues with bowel and bladder; specifically incontinence or difficulty with bowel movements. Performing surgery to remove the uterus certainly would address this.
Abnormal vaginal bleeding
While there are many conservative ways to treat abnormal vaginal bleeding; including medical, hormonal, and other procedures such as ablation, a hysterectomy provides definitive therapy for this issue.
Chronic Pelvic Pain
Hysterectomy for chronic pelvic pain should be an option of last resort as there are many entities for pelvic pain. So many, that a hysterectomy may not treat the underlying cause.
It is very important to undergo a thorough examination and workup by your gynecologist to ensure that this is the correct procedure to treat this particular problem.
Gynecological Cancer
Whether it be cervical cancer, endometrial cancer, or ovarian cancer; a hysterectomy, more commonly, a radical hysterectomy, will be appropriate.
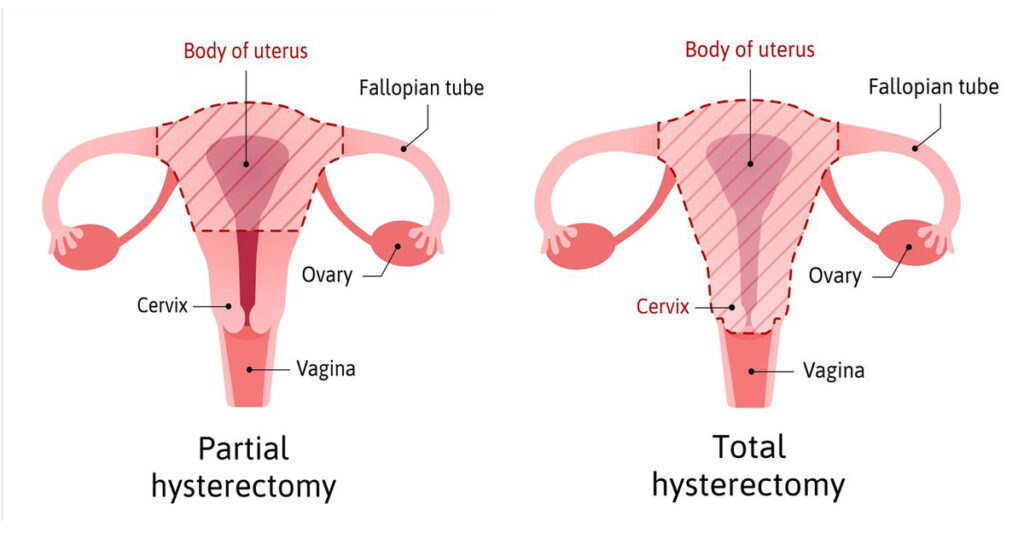
Partial Vs. Complete Hysterectomy
There are many ways to perform a hysterectomy, but before we delve into these, let’s first discuss partial vs. complete hysterectomy.
A partial hysterectomy means that the uterus is removed and the cervix is left behind. This is also commonly referred to as a supracervical hysterectomy.
There are numerous reasons why partial hysterectomies are performed, ranging from a patient request to patient safety.
At the time of surgery, if there is significant scarring, anatomy distortion, etc., precluding safe removal of the cervix, it may be necessary to leave it behind. Women who have partial hysterectomies will still need to be followed with pap smears.
Total hysterectomy means the uterus and cervix are removed. As long as there is no history of abnormal pap smears or gynecological cancers, women undergoing complete hysterectomies no longer need to have pap smears. This does not mean you no longer need to have an annual exam.
Whether or not you have a total (complete) hysterectomy or a partial hysterectomy, nowadays most gynecologists are routinely removing the fallopian tubes at the time of your procedure.
This is called a salpingectomy; bilateral salpingectomy if both tubes are removed.
Research has shown that the precursors for ovarian cancer originate in the fallopian tubes.
Removing or leaving the ovaries at the time of hysterectomy is also known as an oophorectomy, or bilateral oophorectomy (if both ovaries are removed). This conversation is had between the patient and the gynecologist preoperatively, and/or at times can be an intra-op decision.
Types of Hysterectomies
Abdominal Hysterectomy
This is the most common approach. The incision is typically made in the same location as a c-section scar (2 cm above the pubic symphysis). In cases of enlarged uteruses, a vertical incision may be considered.
This is more like your mom’s hysterectomy, meaning, it is what was done back in the days of old. What has been tried and true is still a very popular option.
Most that have an abdominal hysterectomy will be hospitalized for 2-3 days, sometimes longer depending on the postoperative course.
Vaginal hysterectomy
The uterus is removed through an incision made in the vagina. No abdominal are incisions involved. This is considered minimally invasive surgery. If you can find a surgeon that does vaginal surgery; this is a good option to consider.
LAVH (Laparoscopic-Assisted Vaginal Hysterectomy)
While the uterus is still delivered through the vagina, the surgeon utilizes laparoscopic instruments through various ports strategically placed on the patient’s abdomen to take down various ligaments, and blood supply supporting the uterus.
Robotic-Assisted Hysterectomy
This procedure is pretty slick in that it allows the surgeon to perform the hysterectomy while sitting at a console that controls laparoscopic instruments placed in the patient’s abdomen. This is similar to a laparoscopic-assisted vaginal hysterectomy.
The advanced technology allows the surgeon, from the console, to use natural wrist movements to control the laparoscopic instruments while viewing the surgery on a 3-dimensional screen.
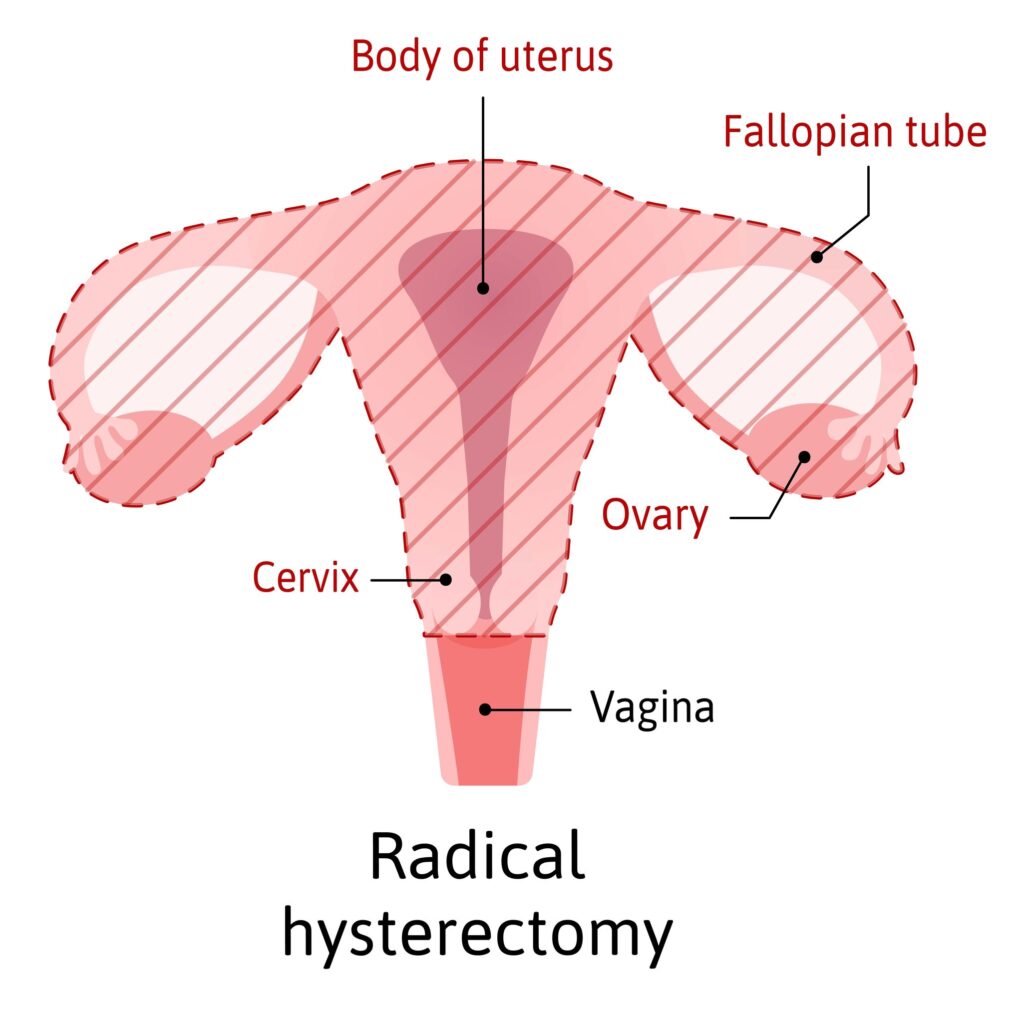
Radical Hysterectomy
This is the type of hysterectomy done in cases where cancer is involved. This hysterectomy is usually done by a Gyn-Oncologist.
With radical hysterectomies, the uterus is removed with wider margins; ie, additional tissue on the sides of the uterus is removed. The cervix as well as a portion of the vagina is removed in radical hysterectomies.
Common Risks Associated With Hysterectomies
Regardless of whether it’s an open or minimally invasive procedure, common risks include but are not limited to the following:
- Bleeding
- Injury to neighboring organs (bowel, bladder, rectum, etc)
- Risk of transfusion
- If done in a minimally invasive fashion; conversion to an open case
- Infection
- Urinary incontinence
- Chronic pelvic pain
The type of hysterectomy you have performed will depend on factors ranging from:
- the indication for the procedure
- pathology involved (cancer for example)
- patient preference
- surgeon experience
- patient qualifications (not every patient is a good candidate for minimally invasive surgery due to history of previous surgeries and ensuing scar tissue and very large uteruses amongst others).
The type of hysterectomy you have performed will also determine the length of your hospital stay. Open procedures such as abdominal hysterectomies often involved a 2 to a 3-day hospital stay.
More minimally invasive approaches such as robotic, laparoscopic, vaginal, etc. may involve an overnight stay or sometimes a day of surgery discharge depending on the postoperative course.
Conclusion
Hoping this blog post has helped address some of the common questions you may have about hysterectomies. If you have further questions, leave them in the comments.
Make sure you sign up for my youtube channel, weekly blog post, and podcast.
Until next time. Choose Happiness.
Dr. Angela, Everyone’s Favorite OBGYN