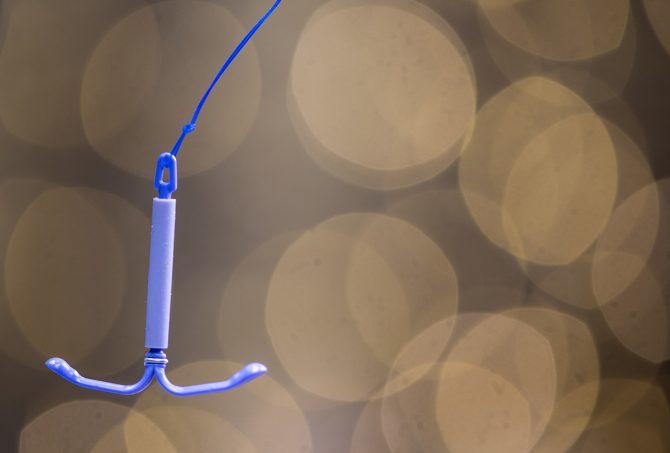
I LOVE IUDs. For those of you not familiar with the abbreviation, IUD stands for intrauterine device. Behind female sterilization and birth control pills, IUDs are the 3rd most popular form of contraception in the United States.
IUDs are T-shaped devices, a little larger than the size of a quarter, that, once placed, sit within the uterine cavity.
They are 99% effective and take user compliance right out of the equation. Once they’re in, they’re in.
They are one of many LARCs (Long-acting Reversible Contraceptives) that are largely responsible for the drastic decrease in teen pregnancy nationwide.
Categories of IUDs
To keep things simple, we’ll divide IUDs into two categories;
- Hormone-releasing, and
- Non-hormone releasing (A.K.A Copper IUDs)
Liletta, Kyleena, Skyla, and Mirena are progesterone-releasing IUDs. Paragard, aka, the Copper IUD, is the non-hormonal IUD. Depending on the type of IUD you have, it can stay in place for 3 to 10 years.
Progesterone releasing IUDs prevent pregnancy by:
- Thickening cervical mucus to prevent sperm from reaching and/or fertilizing an egg
- Making the lining of the uterus unfavorable for implantation via thinning
- Partially suppressing ovulation.
Added benefits of progesterone releasing IUDs include:
- They don’t require partner participation
- They can be removed at any time with a quick return to normal fertility
- They can be used while breastfeeding
- Outside of contraception, they can be used to treat heavy periods. In a nutshell, progesterone thins out the lining of your uterus; hence, you don’t bleed as much when you get your period. On the flip side, irregular bleeding/spotting can be an annoying consequence of progesterone-only types of contraception. Most of the brochures will tell you that post IUD placement, irregular bleeding can last between 3 to 6 months. In my clinical experience, I think it’s closer to 6 to 8 weeks.
The copper IUD (Paragard), prevents pregnancy because the copper material creates a hostile environment for sperm, thus preventing sperm from finding its way to and fertilizing the egg.
Copper IUDs are also highly effective as emergency contraception. If placed within 5 days of unprotected sex, it is > 99% effective in preventing pregnancy. This particular IUD can be associated with heavier, more painful periods.
Here are the most common questions women have been asking.
Is an IUD Right for me?
Most women are candidates for an IUD. If you are in a mutually monogamous relationship and are at low risk for contracting an STI, you are eligible.
However, Contraindications for progesterone releasing IUDs include a history of breast cancer or an increased risk for breast cancer and a history of liver disease.
Contraindications for the copper IUD include allergy to copper or a history of Wilson’s disease.
Do IUD Prevent STIs?
Remember, IUDs do not prevent STIs so it’s important to practice safe sex; i.e, use a condom if you aren’t in a mutually monogamous relationship.
How is an IUD put in?
The setup for placing an IUD is much like a pap smear.
A speculum is inserted into the vagina, and the cervix is visualized and cleansed. I use betadine, to reduce the risk of infection, etc. Then, the IUD is placed.
Placement typically takes no more than 5 minutes. Usually in and out. I typically don’t premeditate with anything other than the NSAID I instruct patients to take prior to insertion.
For women that forget to take it, most still do fine. In my experience, most Ob-Gyns do not provide pain relief for IUD insertion. Although, the literature is inconclusive on whether or not administering some sort of anesthetic for insertion is helpful.
Is IUD placement REALLY that bad?
It depends.
In my reading, I recently came across an article discussing the pain associated with IUD insertion and doctors not giving women a “heads up,” so to speak.
As I always say, in my best GI Joe voice, “knowing is half the battle.”
When women know what to expect leading up to having their IUDs placed, I feel as if it goes a lot smoother. You’ve taken anticipation and anxiety right off the table.
I instruct all of my patients to take some sort of non-steroidal 30 minutes prior to insertion; these include meds such as Motrin, Ibuprofen, Alleve, etc.
This helps with cramping; the most common symptom experienced with placement. I prefer to insert IUDs when a woman is on the tail end of her period. That way, the cervix is already open. I find that it makes placement easier. For the record, you do not have to be on your period to have an IUD placed.
It’s really important to listen to your patient and acknowledge their feelings. On occasion, I have had patients become light-headed, dizzy, or extremely uncomfortable post-insertion.
This is nothing that a cold compress to the forehead or back of the neck, a glass of water, and reassurance won’t fix.
I would not be opposed to using a local agent such as Lidocaine(a local anesthetic) if the patient requested it or was really nervous. Something like a Paracervical block, the type of anesthesia used for most in-office leep procedures, could be of use on such occasions.
Again, the big thing is making sure that the patient is aware of what to expect before, after, and even during the procedure.
I would LOVE to hear from you, specifically if you have or had an experience with an IUD. Did you like it? How was your insertion experience?
Until next time,
Choose Happiness.
Dr. Angela